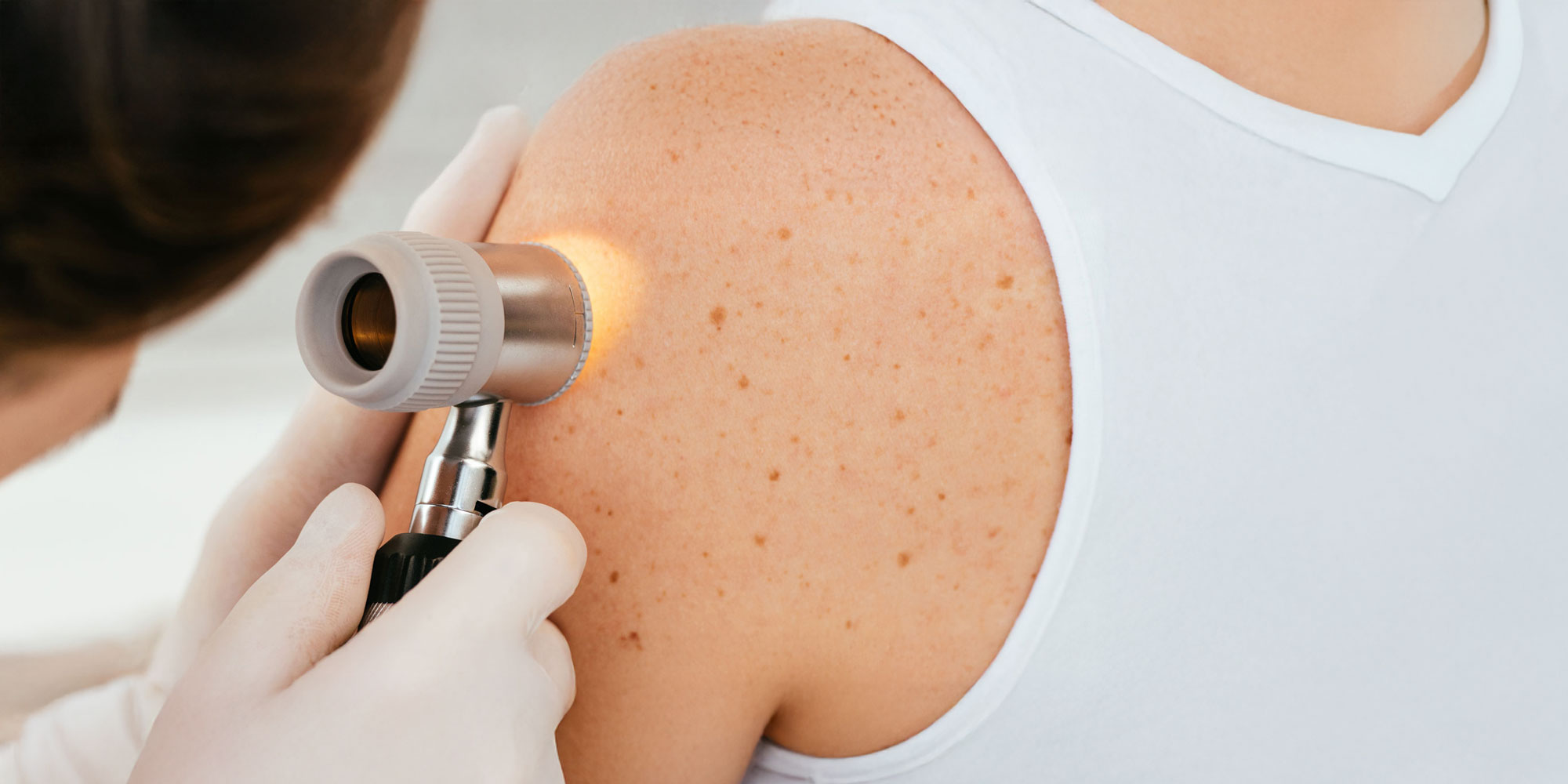
If you or a loved one was diagnosed with melanoma, you deserve expert care that’s close to home. Melanoma is a type of skin cancer that begins in melanocytes, the cells responsible for producing melanin, the pigment that gives skin its color. While it is less common than other skin cancers like basal cell carcinoma or squamous cell carcinoma, melanoma is more aggressive and more likely to spread to other parts of the body if not caught early. Melanoma can occur anywhere on the body but is most commonly found on the back, legs, arms, and face.
There are several subtypes of melanoma:
-
Superficial spreading melanoma: The most common form, often appearing as a flat or slightly raised discolored patch with irregular borders.
-
Nodular melanoma: A more aggressive subtype that often grows more quickly and appears as a bump on the skin.
-
Lentigo maligna melanoma: Typically found in older adults, often on sun-damaged skin such as the face.
-
Acral lentiginous melanoma: A rarer form, usually found on the palms, soles, or under the nails, is more common in people with darker skin.
Desmoplastic melanoma: An uncommon type that tends to occur on sun-exposed areas and can be challenging to diagnose.
Early Stage Survival Rates for Melanoma
When detected early, melanoma is highly treatable. The five-year survival rate for people with melanoma that is confined to the skin (localized stage) is about 99%. These high survival rates underscore the importance of early detection and timely treatment decisions. Regular skin checks and prompt evaluation of new or changing moles can be life-saving. The later melanoma is diagnosed, the more difficult it is to completely cure.
Stages of Melanoma
The overall stage of melanoma ranges from Stage 0 (in situ, confined to the top layer of skin) to Stage IV (metastatic melanoma that has spread to distant organs):
- T (Tumor): Describes the thickness of the melanoma and whether the skin is ulcerated.
- N (Nodes): Indicates if melanoma has spread to nearby lymph nodes.
- M (Metastasis): Identifies whether the cancer has spread to distant organs.
Melanoma stages range from 0 to IV:
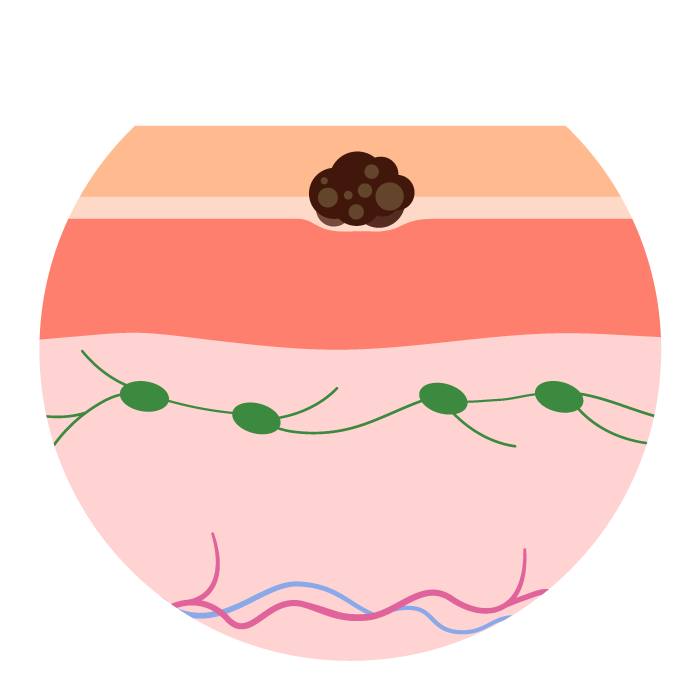
Stage 0 (Melanoma in situ) Tis, N0, M0:
Melanoma is confined to the outermost layer of the skin (epidermis) and has not penetrated deeper. There is no lymph node involvement or metastasis.
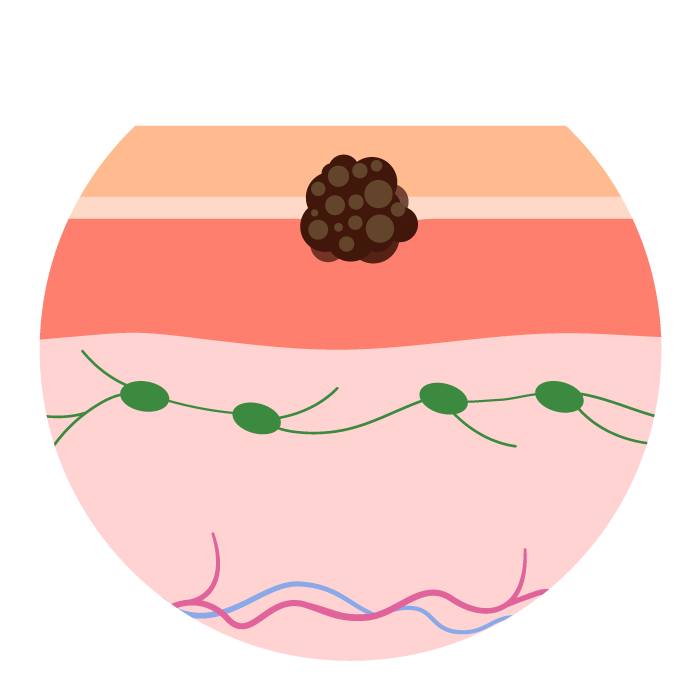
Stage I (T1–T2a, N0, M0):
The tumor is up to 2mm thick. There is no spread to lymph nodes (N0) or distant sites (M0).
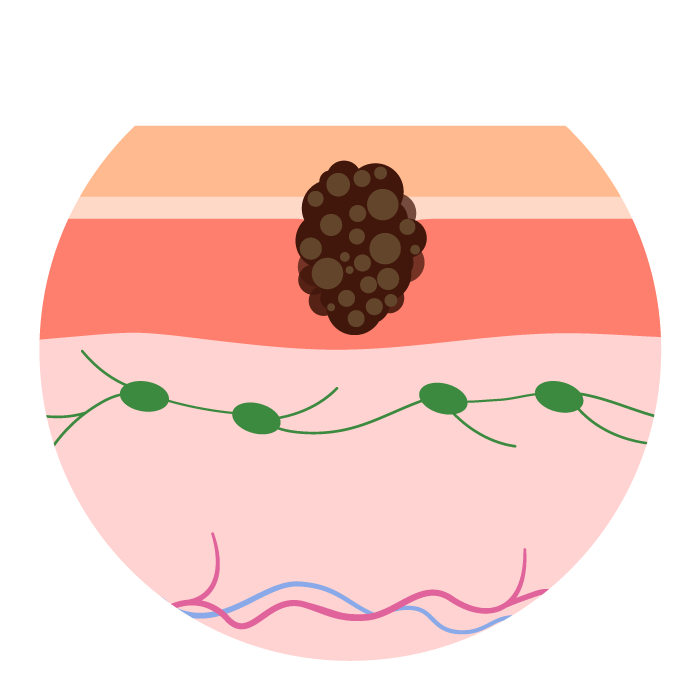
Stage II (T2b–T4b, N0, M0):
The tumor is more than 2 mm thick and ulcerated or more than 2 mm thick with or without ulceration. It still has not spread to nearby lymph nodes (N0) or distant parts of the body (M0).
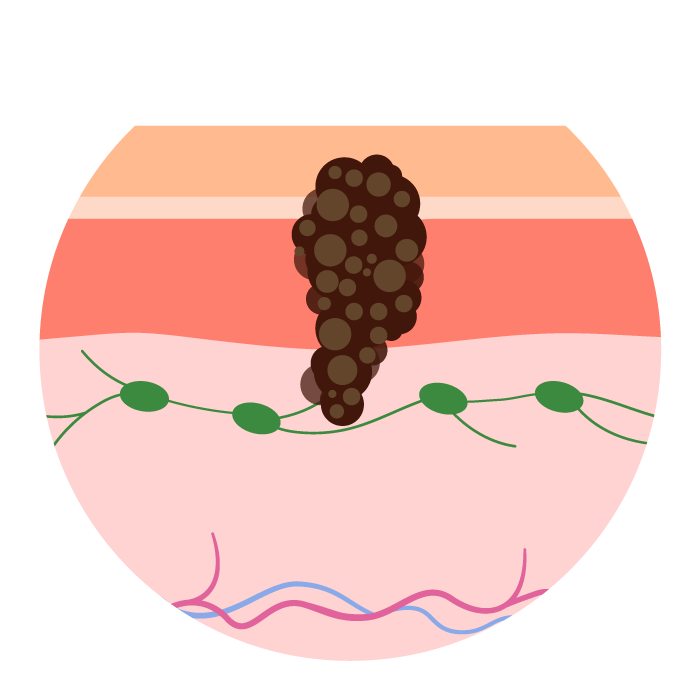
Stage III (Any T, N1–N3, M0):
Melanoma may be of any thickness and might be ulcerated. It has spread to one or more nearby lymph nodes or to small areas of nearby skin or lymph vessels (N1–N3). There is no distant metastasis (M0).
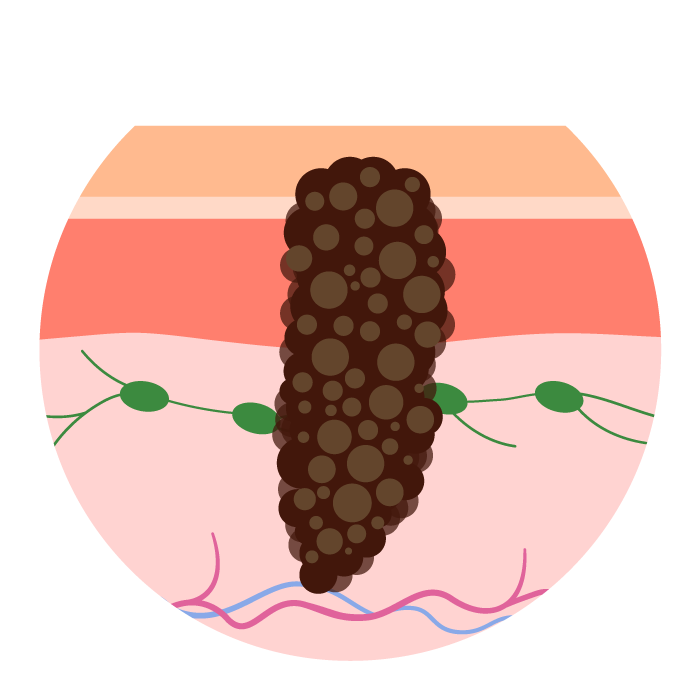
Stage IV (TNM: Any T, Any N, M1):
The melanoma has spread to distant organs such as the lungs, liver, brain, or to distant skin and lymph nodes, regardless of tumor thickness or lymph node involvement.
Treatment Options for Melanoma
Melanoma treatment is highly individualized and depends on the stage of the disease and the tumor’s genetic characteristics. Our team at Shenandoah Oncology collaborates closely with the dermatologist and surgeon to design a treatment plan that fits your unique situation. Treatment options may include:
Melanoma Surgery
Surgery is the primary treatment for early-stage melanoma. For some early-stage melanomas, surgery may be the only treatment necessary. The dermatologist or a surgeon who specializes in skin cancer will select the surgical method that’s best for each patient based on the cancer’s size and how deeply it has penetrated into the skin layers. For those with later-stage melanoma, additional treatments may be recommended after surgery to be sure all of the cancer cells are destroyed.
Immunotherapy for Melanoma
For advanced or metastatic melanoma, immunotherapy is a key treatment option that helps the immune system more effectively recognize and destroy cancer cells. It works by blocking proteins like PD-1 and CTLA-4 — known as immune checkpoints — that normally suppress immune responses. By inhibiting these checkpoints, T-cells, a type of immune cell, are unleashed to attack melanoma cells more aggressively, leading to improved outcomes in many patients.
These treatments can be given alone or in combination, depending on factors such as disease progression, side effects, and overall health. Combination therapies often produce stronger responses but can also increase the risk of immune-related side effects. Immunotherapy is typically given intravenously every few weeks, and treatment duration depends on stage, tolerance, and response.
Targeted Therapy for Melanoma
Melanoma tumors with specific genetic mutations, such as BRAF mutations, may respond to targeted therapy. These drugs block abnormal growth signals in cancer cells and are often used together for greater effectiveness. Your oncologist will run biomarker tests on the cancer to see if targeted therapy is right for you.
Melanoma Radiation Therapy
Radiation therapy uses high-energy rays to destroy cancer cells. For melanoma, it is not typically the first treatment option, but it can be used in a few different ways:
-
After surgery, especially if cancer there is a high risk of recurrence.
-
After surgery, to treat the area where lymph nodes were removed.
-
To relieve pain caused by melanoma that has spread to other areas of the body, such as the brain or bones.
For patients who cannot undergo surgery due to other health conditions, radiation may be used as the primary treatment.
Chemotherapy
Chemotherapy uses drugs to kill cancer cells and may be administered by mouth or through an IV. While it is less commonly used today because of advances in immunotherapy and targeted therapy, chemotherapy may still be considered in certain advanced melanoma cases.
Clinical Trials
Participation in clinical trials may offer access to new therapies that are not yet widely available. Shenandoah Oncology provides patients with the opportunity to participate in these trials, which may include innovative immunotherapies, vaccines, or combination treatments.