Colorectal Cancer Care at Shenandoah Oncology
Colorectal cancer is a collective term for two gastrointestinal cancers: cancer that begins in the colon and cancer that begins in the rectum. Together they’re referred to as colorectal cancer. The most common type is adenocarcinoma, which starts in mucus-producing cells lining the colon or rectum.
The experienced Shenandoah Oncology team reviews each patient’s specific needs to create a personalized treatment plan based on the size of the cancer, lymph node involvement, the cancer’s genetic profile, and the patient’s personal preferences. Our cancer center in Winchester, Virginia, offers the most advanced colon and rectal cancer treatments, including access to clinical trials.
How Colorectal Cancer Is Diagnosed
Diagnostic Tests for Colorectal Cancer
If screening or symptoms suggest an area of concern, the next step typically involves a gastroenterologist or colorectal surgeon performing a colonoscopy with a biopsy. They will remove either an entire polyp or an area of concern inside the colon to be tested for cancer.
If cancer is confirmed, imaging tests are used to scan the colon and surrounding area for signs of cancer that has grown in other areas.
-
For more advanced assessment or restaging if cancer has recurred, a PET‑CT scan may be used to look for cancer in distant areas of the body, even if it has not yet formed a tumor.
-
Biomarker (molecular) testing on tumor tissue helps tailor targeted therapy or immunotherapy options.
What Are the Stages of Colorectal Cancer?
Staging determines how far the cancer has spread and is fundamental in guiding treatment. Shenandoah Oncology uses detailed staging derived from the TNM system developed by the American Joint Committee on Cancer (AJCC). The TNM system includes:
- T (Tumor): how deeply the tumor has invaded the colon/rectal wall.
- N (Nodes): whether cancer has spread to nearby lymph nodes.
- M (Metastasis): whether it has spread to distant organs.
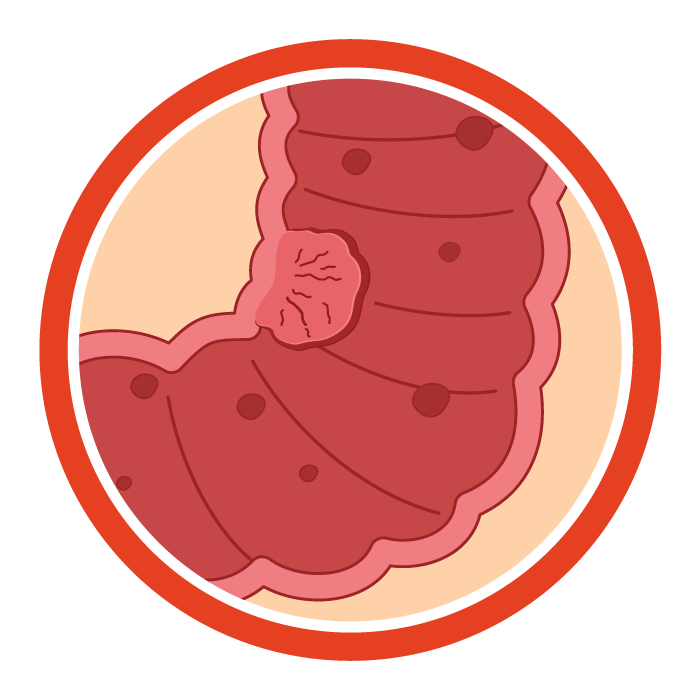
Stage 0 (Tis N0 M0):
Carcinoma in situ—tumor confined to the innermost layer.
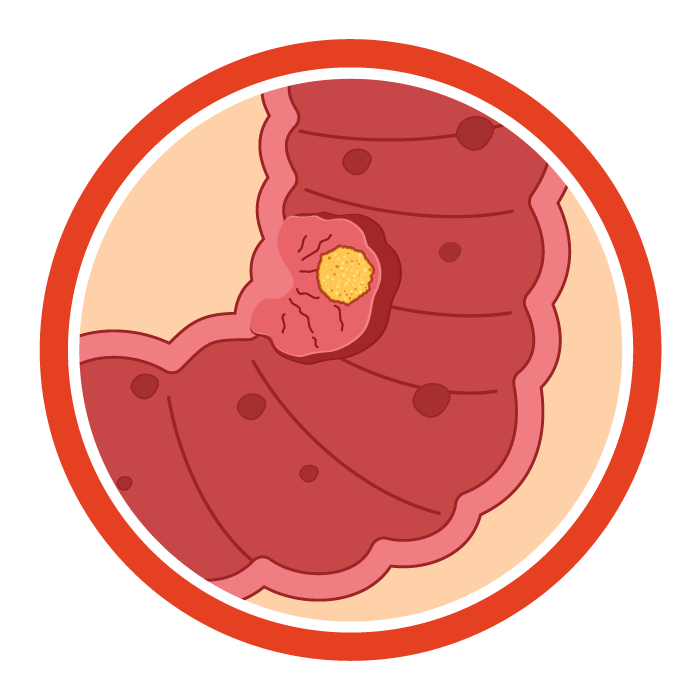
Stage I (T1–T2 N0 M0):
Tumor invades submucosa or muscle layer only. No lymph nodes are affected.
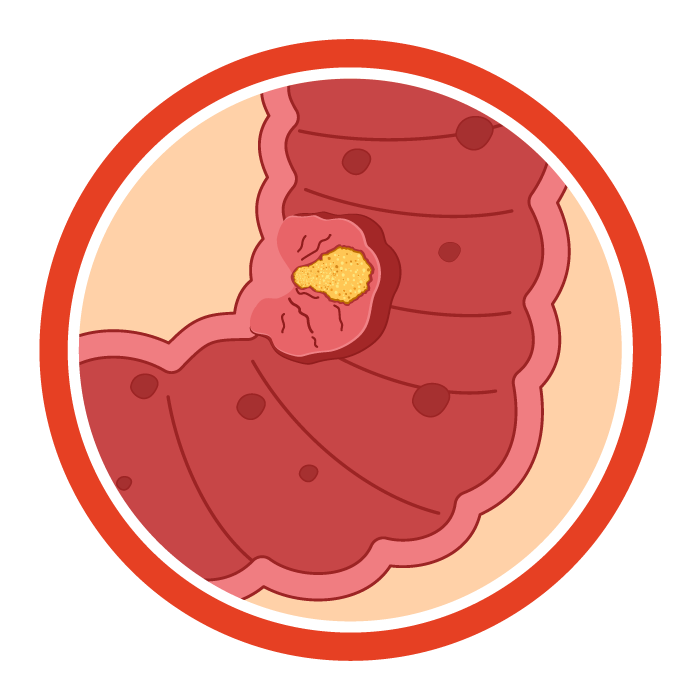
Stage II (T3-4 N0 M0):
-
The cancer has grown through the wall of the colon or rectum and may have reached nearby tissues, but it has not spread to any lymph nodes or distant organs.
-
Stage IIA: Cancer has grown through the wall of the colon and into the tissues around the colon. There is no lymph node involvement.
-
Stage IIB: Cancer has grown through the wall of the colon and invades a layer called the visceral peritoneum. There is no lymph node involvement.
- Stage IIC: Cancer has grown through the wall of the colon and directly invades or adheres to adjacent organs or structures. There is no lymph node involvement.
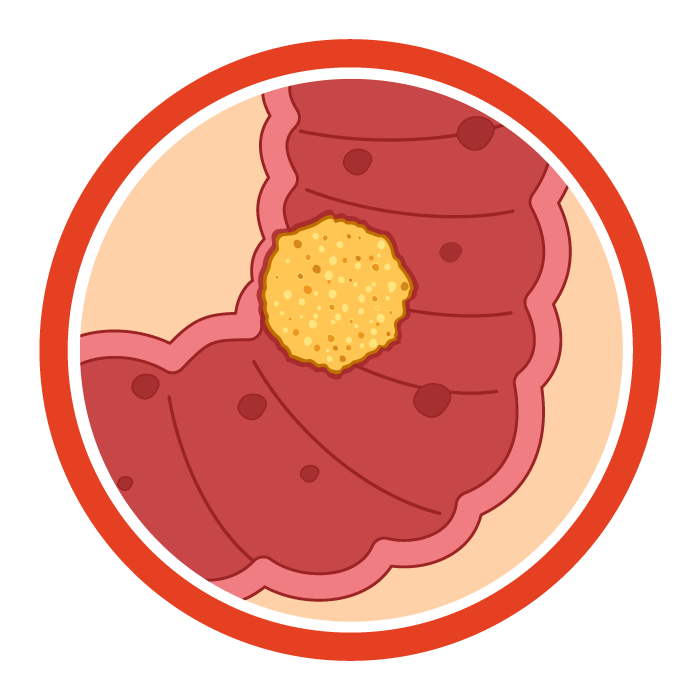
Stage III:
-
The cancer has spread to nearby lymph nodes but has not reached distant parts of the body. How far it has spread into the colon or rectum wall and the number of lymph nodes affected varies by substage.
-
Stage IIIA: The tumor has grown deeper into the colon wall but not necessarily all the way through. Lymph node involvement is limited (no more than 6 nearby/regional lymph nodes).
-
Stage IIIB: Larger tumors or more extensive local spread, with lymph node involvement.
- Stage IIIC: The tumor has grown to the outermost layer of the colon or through the colon wall. More lymph nodes are affected.
Stage IV (any T, any N, M1):
Distant spread, such as to the liver or lungs; subcategories M1a, M1b, M1c define single vs multiple sites of spread.
Staging is important for your oncologist to make decisions about treatment plans, prognostic expectations, and whether additional therapies like targeted therapy, radiation, and other cancer treatments are necessary before or after surgery.
Treatments for Colorectal Cancer
A multidisciplinary team, including the medical oncologist, radiation oncologist, and surgeon, coordinates and discusses the best treatment options for each patient. The medical oncologist typically leads the team and meets with patients to provide personalized colorectal cancer treatment plans.
Surgical Approaches for Colorectal Cancer
-
For Stage 0–I, many colon cancers are treated with local excision of a polyp that has become cancerous, or a partial colectomy. Rectal cancers often require surgical resection, sometimes with chemoradiation before surgery to shrink the tumor and improve outcomes.
-
In more advanced Stage II and III disease, surgery is combined with lymph node removal and may be preceded or followed by systemic or radiation therapies depending on tumor location.
-
Stage IV colorectal cancer treatment does not usually include surgery. It may be considered if the tumor is causing a lot of symptoms or if there is concern that the tumor will cause a complete obstruction.
Chemotherapy for Colorectal Cancer
-
Chemotherapy (typically over three to six months) is recommended for Stage III colon cancer and considered in high-risk Stage II cases. For colorectal cancer, a combination of chemotherapy drugs is most effective.
-
For Stage IV, systemic chemotherapy may be given before surgery (neoadjuvant), after surgery to destroy any cancer cells that remain in the lymph nodes and other organs, or as palliative therapy to relieve pain, control disease and prolong life.
Immunotherapy for Colorectal Cancer
The immune system has natural safeguards that prevent it from attacking healthy cells. These safeguards include “checkpoints,” which are proteins on immune cells that need to be activated—or turned off—at the right time to trigger an immune response. Some colorectal cancer cells have learned how to trick these checkpoints, allowing them to escape being attacked by the immune system.
Checkpoint inhibitors are a category of immunotherapy that allows the immune system to identify and destroy cancer cells. By blocking the checkpoint proteins, these medications reactivate the immune system.
At Shenandoah Oncology, we use checkpoint inhibitors when genetic testing shows that a colorectal tumor has specific features such as a high level of microsatellite instability (MSI-H) or mutations in mismatch repair (MMR) genes. They are often administered as the primary treatment or at the same time as chemotherapy.
Targeted Therapy for Advanced Colorectal Cancer
If your cancer is found to be advanced, we will send your biopsy or surgical specimen for additional testing. If a particular genetic change is detected, specific targeted therapies, usually along with chemotherapy, can be used to target and destroy cells with the mutation. For metastatic colorectal cancer, treatment may include targeted therapies that address specific issues found in the patient’s biomarker testing results, such as:
-
VEGF protein overgrows, which supports blood vessel development. By cutting off the blood supply to the cancer cells, they are unable to reproduce.
-
Genetic changes to genes, including BRAF, RET, NTRK, or KRAS (with others under extensive research).
-
HER2 and EGFR protein overgrowth caused by a genetic change that supports cancer cell growth.
Radiation Therapy
This treatment is primarily used for rectal cancer, often combined with chemotherapy before surgery to reduce tumor size and lower recurrence risk. It can also be used after surgery in some instances, especially for colon cancer that has attached to another organ or to reduce symptoms of advanced colon cancer, such as a tumor causing a colon blockage, bleeding, or pain.
Colorectal Cancer Clinical Trials
Cancer research is the reason we have the treatments we do today. Shenandoah Oncology is pleased to participate in clinical research trials that bring the most recent therapies to our patients. If you are a candidate for a clinical research trial for your specific type and stage of colorectal cancer, our research team will discuss participation with you. Feel free to ask about the pros and cons of participating in the trial and your other options if you choose not to participate.




